Estimated reading time: 13 minutes
It stated a few days after my first injection. A strong, persistent fullness. A wave of nausea that arrived without warning and stayed for days. A body that suddenly had strong opinions about everything I tried to eat. And then, just when I thought I had found my footing, I increased my dose, and the whole adjustment started over. That’s when I realized I could use the Mediterranean diet to Manage the Ozempic Gut.
If any of that rings a bell, you’re in good company. About one in four people on GLP-1 therapy go through this awkward digestive phase. But, here’s what doesn’t get said enough: it’s manageable. And for most of us, it gets a whole lot better as the months go by and your body finds its new groove.
What actually helps isn’t some magic supplement, or a strict set of rules. It’s a gentler, more forgiving way of eating, one that’s been part of Mediterranean kitchens for generations. This guide walks you through what’s happening in your body and how are you few Mediterranean habits can help you feel more comfortable, one meal at a time.
How to Manage the Ozempic Gut With Mediterranean Ease
Table of contents
- What is Happening in Your Digestive System
- Simple Mediterranean Habits That Help You Manage the Ozempic Gut
- Building Your Fiber Foundation to Manage the Ozempic Gut
- Hydration Rituals that Help You Manage the Ozempic Gut
- Culinary Pacing to Manage the Ozempic Gut More Comfortably
- Natural Remedies to Help You Manage the Ozempic Gut
- Foods to Avoid to Help You Manage the Ozempic Gut
- Better Days Are Coming
- Frequently Asked Questions About How to Manage the Ozempic Gut
Welcome back to the table. This is week three of my Mediterranean eating starter series. If you are just joining the conversation, I highly recommend catching up on my first two articles. You can read The Mediterranean Diet for GLP-1 Nausea: How I Eat to Feel Better and Lose Weight and Mediterranean Protein Guide for GLP-1 Users to get the full story on how I started this journey.
Fourteen months in, I can tell you honestly: those first few days after each shot are still the hardest part of my week. But, they are manageable now in a way they weren’t at the beginning. And, the difference had almost nothing to do with willpower or discipline. It had everything to do with learning how to eat for the body I was living in. Not the one I had before.
If you are navigating this right now, whether it is your first week or your fifth dose increase, this guid is what I wish someone had handed me on day one.
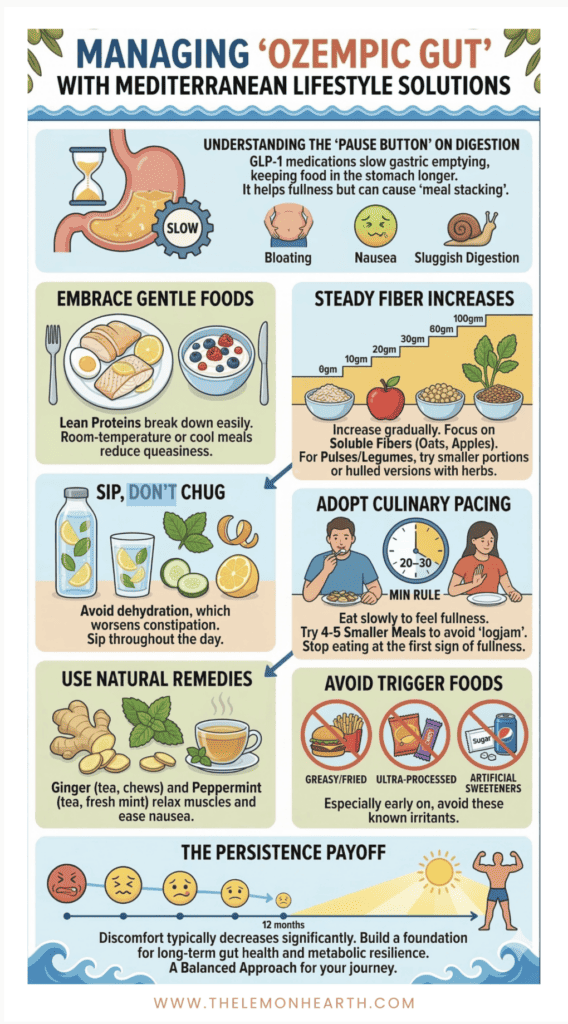
What is Happening in Your Digestive System
Understanding how gastric emptying slows makes it much easier to manage the Ozempic Gut with patience and a little strategy. GLP-1 medications work, in part, by slowing gastric emptying. That is the clinical term for the rate at which food moves from your stomach into your small intestine.
That slower paces is actually part of how these meds work. You stay fuller longer, your appetite dials downs and weight loss feels a bit steadier. But, it also measures your digestive system is running on a new timeline.
Before medication, your stomach would bounce back from a meal in just a few hours. Now, that window stretches out. If you eat lunch before your breakfast has finished its journey, you might feel pretty uncomfortable. The results are a familiar cluster of symptoms.
- Nausea, especially the days after your shot
- Bloating and a sense of fullness that lingers
- Sluggish digestion
- General feeling that your stomach is working on a schedule you did not agree to
None of this means something is wrong. Your body is just learning a new rhythm. The trick is to eat in a way that aligns with that rhythm, rather than fighting it.
How I Manage the Ozempic Gut
Before we get into the full framework, I want to share what works for me personally, because I think it matters more than any general advice.
On the three to four days after my shot when nausea is at its worst, I let go of the idea of eating meals entirely. Instead, I make something calorie-dense, high in healthy fats and easy to eat in small amounts through out the morning. My go-to is a chia pudding made with full-fat Greek yogurt, high-protein milk, fruit, and a little honey. Around 692 calories in a small jar. I eat a few spoonfuls every two hours, and I sip water consistently through the day; usually around three liters.
That shift alone changed everything for me. Small. Calorie-dense. High in healthy fats. No pressure to finish.
If you want a structured version of this approach for those first post-shot days, my Mini-Meal Builder was built for exactly that window. It takes the guesswork out of what to eat when eating feels hard.
Simple Mediterranean Habits That Help You Manage the Ozempic Gut
When your digestion slows down, what you eat suddenly matters a lot more. The good news? The Mediterranean diet is already built around foods that are easy on your system. Simple, whole, and nourishing, without weighing you down.
During those early weeks or after a dose bump, these are the foods that usually go down easiest.

Mediterranean Staples That Help You Manager the Ozempic Gut
Heavier meats can hang around in your stomach longer than you’d like, especially when things are moving slowly. Lighter proteins are much kinder to your system.
- Poached or baked chicken breast
- White fish such as cod or tilapia
- Eggs, prepared simply
- Greek yogurt, plain and unsweetened
- Chia seed pudding

Cool or Room-Temperature Meals for GPL-1 Comfort
On days when your stomach is feeling sensitive, strong smells or hot, heavy foods can turn your appetite right off. Cold, or room-temperature meals are often much easier to handle.
- Greek yogurt bowls with fruit and a drizzle of honey
- Cold grain salads with cucumber, herbs, and olive oil
- Room-temperature lentil dishes
- Chilled vegetable soups
Bland Mediterranean Grains for Slower Digestion
Plain carbs can be surprisingly comforting, no stress, just something gentle for your gut.
- Plain brown or white rice
- Oats with minimal toppings
- Plain crackers
- Barley cooked soft
Building Your Fiber Foundation to Manage the Ozempic Gut
Fiber is your gut’s best friend, just not all at once. On GLP-1 therapy, adding too much too fast can leave you feeling gassy, bloated, and generally uncomfortable.
The approach that works is not to avoid fiber. It’s to build it slowly and deliberately.
I add chia seeds, hemp seeds, and flaxseed to my Greek yogurt every single day. But, I didn’t start with all three at once. I introduced them over several weeks, giving my gut time to adjust before adding more.
Start with Soluble Fiber
Starting with soluble fiber is one of the most reliable ways to manage the Ozempic Gut while still nourishing your microbiome. Soluble fiber is the gentle starter. It dissolves in water and forms a soft gel, moving through your system without causing drama. It’s the easiest place to begin.
- Oats
- Barley
- Apples, peeled
- Peaches
- Carrots, cooked soft
Chickpeas and Legumes Without the Bloat
Approach legumes carefully. Chickpeas and lentils are cornerstones of Mediterranean eating and excellent sources of both fiber and plant protein. If they cause bloating, start with two or three tablespoons rather than a full serving. Choose hulled or red lentils over whole green varieties, rice canned chickpeas thoroughly and pair them with digestive herbs like mint, parsley, or cumin.
The Gradual Rule for GLP-1 Digestion
Give your gut time. Increase fiber by just a few grams every few days. Rushing this is one of the most common causes of unnecessary discomfort on GLP-1 therapy.

Hydration Rituals that Help You Manage the Ozempic Gut
GLP-1 medications can quiet your thirst signals. Even a little dehydration can make constipation and discomfort worse. You don’t need to chug a big glass of water at every meal. In fact, that can make your feel even fuller or nauseas. The real goal is to sip steadily, keeping things gentle all day long. Steady hydration is a quiet but powerful tool to manage the Ozempic Gut, especially when thirst cues are muted.
For myself, I drink three liters of water a day. This works for me because I live in south Texas; a place that is hot and humid most of the year. It may sound like a lot, but, when I spread it across the entire day, it becomes natural.
Mediterranean Hydration Infusions
If plain water feels unappealing on nauseous days, Mediterranean-inspired infusions make hydration something you can look forward to. You can try:
- Lemon slices with mint, cucumber, and basil
- Orange peel with fresh ginger
- Warm water with a slice of lemon
They’re gentle, they work, and they turn hydration into a little daily ritual you might even enjoy.
Culinary Pacing to Manage the Ozempic Gut More Comfortably
Mediterranean food culture has always understood something that modern eating habits tend to ignore. Meals are ment to be experienced, not rushed through. Turns out, that philosophy is genuinely helpful when you’re on a GLP-1.
The 20 to 30 Minute Rule
Eating slowly gives your brain a chance to catch up with your stomach before you hit the wall. ON a GLP-1, those signals are even more sensitive. If you eat too fast, you may not realize you’re full until it’s too late, and then you’re stuck feeling uncomfortable. Aim for 20 to 30 minutes per meal. Put your fork down between bites. Try to eat at a table, not hunched over your laptop.
Smaller, More Frequent Meals for GLP-1 Ease
A lot of people feel better on a GLP-1 by swapping big meals for four or five smaller ones. It helps keep meals from pilling up on each other and causing trouble. You don’t need to get fancy with mini-meals. A small bowl of yogurt with fruit, a handful of walnuts, an apple, or a few crackers with hummus is simple, satisfying, and easy on your system.
The Satiety Stop Sign
One of the best habits you can build on a GLP-1 is stopping as soon as you feel full. Not almost full, actually full.. That last bite you used to take without thinking? Now it can stick with you for hours. Learning to spot your new fullness cues and actually listening to them is one of the best ways to keep yourself comfortable.
Natural Remedies to Help You Manage the Ozempic Gut
Before you reach for medication, take a look at the Mediterranean pantry. Both ginger and peppermint are classic Mediterranean remedies that can help you manage the Ozempic Gut with gentle, everyday support.
Ginger for Nausea and Slow Digestion
Ginger has been a go-to for nausea and digestion for centuries. It helps relax your digestive tract and gets things moving again. When GLP-1 slows everything down, ginger can be a real lifesaver.
- Ginger tea, steeped for five minutes
- Ginger chews or lozenges, kept in your bag for on-the-go releaf
- Fresh ginger grated into warm water with lemon
- A simple lemon ginger broth
Peppermint for Bloating and Cramping
Peppermint helps relax your gut muscles, which means less cramping, less bloating, and less of that post-meal pressure.
- Peppermint tea after meals
- Fresh mint leaves added to water throughout the day
- Mint salads
These remedies are gentle enough to use every day and fit right in with Mediterranean eating.
- Peppermint. Helps reduce cramping, bloating, and pressure.
- Peppermint tea
- Fresh mint leaves in your water
- Mint-forward salads
Foods to Avoid to Help You Manage the Ozempic Gut
You don’t need a laundry list of rules. But, there are a few types of food that almost always make GLP-1 digestive symptoms worse, especially in those first weeks after a dose increase.
Ultra-Processed Foods
Highly processed foods can ramp up inflammation, mess with your fullness signals, and make slow digestion even more uncomfortable. And, they are engineered to override your fullness cues. Skipping them helps both your comfort and your long-term goals.
Greasy or Fried Foods
Fat slows things down even more. When you mix greasy foods with a GLP-1, you can end up with course of discomfort or nausea even from foods you used to handle just fine.
Artificial Sweeteners
Sweeteners like sorbitol and xylitol are famous for causing bloating and gas. Check the labels on low-calorie snacks and protein bars; they snack in everywhere.
Better Days Are Coming
If you’re in the thick of it right now, here’s what I want you to hold on to.
Your body is not broken. it is adapting. And, the habits you are building right now, eating gently, hydrating steadily, slowing down at the table, are not coping strategies. They are the foundation of a genuinely different relationship with food.
If you want a calm, structured way to reset your eating rhythm during this season, my Mediterranean Refresh was designed for exactly this. It’s not a diet or a detox. It’s a clear framework for eating in a way that works with your medication and your body.
The Mediterranean way was never about restriction. It was about rhythm, pleasure and care. That is exactly what this season calls for. Adopting a Mediterranean diet for GLP-1 nausea was the turning point for me in making this journey feel like a lifestyle rather than a struggle.
Frequently Asked Questions About How to Manage the Ozempic Gut
These Mediterranean habits are some of the most effective ways people naturally manage the Ozempic Gut while their bodies adjust.
it’s the digestive changes some people experience on GLP-1s. It includes early fullness, nausea, bloating, and slower digestion. All are connected to the medication’s effect on gastric emptying; the rate of food moving through your stomach.
Slowing gastric emptying is one of the intended effects of the therapy. It helps reduce appetite and supports weight loss. The discomfort comes when meals are eaten too closely together and the system gets backed up.
Poached chicken, white fish, eggs, plain oats or brown rice. Chilled Greek Yogurt and room-temperature salads.
Slowly. Add just a few grams every few days and give your gut microbiome time to adjust. Start with soluble fiber sources like oats, barley and soft-cooked vegetables before moving to higher-fiber legumes. If lentils or chickpeas cause issues, start with smaller portions and hulled varieties.
GLP-1 medications can reduce your thirst signals, making it easy to under-hydrate without realizing it. Dehydration directly worsens constipation and digestive discomfort. Sipping water consistently throughout the day, rather than in large amounts at once, is the most effective approach.
For most people, yes. Shifting to four or five smaller meals rather than two or three larger ones prevents the stacking effect that causes discomfort. Slowing down while eating also gives your body time to register fullness before you overshoot it.
Ginger and peppermint are both well-supported by research and are natural fits within Mediterranean eating. Ginger tea, ginger chews, peppermint tea and fresh mint in water are all gentle, effective and easy to incorporate daily.
The three categories that consistently worsen symptoms are ultra-processed foods, greasy or fried foods and products with artificial sweeteners. Reducing these during the first weeks and after dose increases makes a noticeable difference for most people.
Eat gently. Sip slowly. Give yourself time.
medical disclaimer
I share this post to provide helpful information and educational resources based on my own experiences and research. However, it’s important to remember that everyone’s health needs are unique, and this content is not a substitute for professional medical advice. If you’re considering any changes to your diet, supplements, or overall health routine, I strongly recommend consulting with your doctor or a qualified health professional first. They can offer personalized guidance based on your individual health history and needs.